Can the Fully Ruptured ACL Heal Itself?
- Tim Trevail
- Oct 27, 2022
- 5 min read
Last updated: October 2022
A review of the current evidence.
If you've been following the Anterior Cruciate Ligament (ACL) news in recent years, you'd likely be aware of the hot topic that is the spontaneous self-healing of the ligament after a complete rupture. This blog reviews the following assumptions:
The ACL cannot heal without surgery
Without surgery, the ACL-deficient knee will be inherently unstable
For a long time, it's been a commonly held assumption that the ACL cannot heal once fully ruptured. It's thought that ACL healing capacity is limited by a lack of ability for blood clots and scaffolding between two ruptured ends of the ligament and a layer of synovial tissue forming over the ruptured ACL endpoints that prevent the ends from coming together again. This belief is part of the reason ACL surgery has been commonplace as the first-line gold standard option for so many years.
ACL reconstruction is one of the most commonly performed surgical procedures worldwide, with very good results in terms of restoring knee stability, recovery of function, and return to sports at a preinjury level... but is it actually a necessary cost to return to function?!
In recent years, non-surgical approaches have gained in popularity. I've previously blogged on whether surgery is needed after an ACL injury. That blog discussed a range of considerations as to whether surgery might be the right option for you. This blog recognised that not all Anterior Cruciate Ligament (ACL) injuries require reconstructive surgery and that many people can return to high-level activities and cope well without an ACL.
Evidence appears to be building that full-thickness ACL tears may have the ability to heal, putting further weight to the non-surgical options for ACL treatment.
Let's have a look at the evidence...
What's the evidence for self-healing ACLs?
The first study to suggest spontaneous self-healing ACLs was way back in 1994. Ihara et al. (1994) looked arthroscopically (surgically with cameras) at combined meniscal and ACL injury 3- months after the initial injury, and found that 20 of the 25 ACL injuries had healed significantly. It's not clear whether these were full ligament ruptures, but important to first demonstrate the healing capacity of this ligament.
Fujimoto et al (2002) took 31 people with ACL ruptures and put them in an extension knee brace for 3 months. 8 participants later underwent surgery due to ongoing instability. Of the remaining 23, 21 were found to have significant healing on MRI.
Fujimoto et al. (2002)
Costa-Paz et al. (2012) shared their observations that an acutely injured ACL may eventually spontaneously heal without using an extension brace, allowing a return to athletic activity. They looked at 14 active people, testing at point of injury and 2 years after ACL rupture. They found that all 14 showed end-to-end continuous ACL. Importantly, all athletes returned to the same or almost the same physical activity as before the injury with normal, or near-normal, strength and function. The authors note that 2 of the 14 did go on to re-rupture the ACL within 2 1/2 years and went on to get surgery. They also speculate that there may be few fibres in continuity not shown in the MRI studies, and overlying synovial lining holding the ends in proximity might have influenced the spontaneous healing.
Ihara and Kawano (2017) looked at how age impacts the healing ability of the ACL and found that younger demographics had more significant injuries, suggesting that it may be less likely for the ligament to spontaneously heal through rehabilitation and time alone.
The Filbay et al (2021) data demonstrated that 56% of people enrolled in a rehab-alone group had a healed ACL 2 years after the initial injury. This is really exciting data, but we should take this with caution as it's preliminary data based on a small sample (n=26).
How does the ACL actually heal?
Study of the ligament suggests that the ACL does in fact, have the biological plausibility and potential to heal. When a ligament is torn, it forms a platlet clot in the area, which attracts mesenchymal (stem) cells in large numbers that morph into the cells that lay down new collagen tissue which the ligament is primarily made from.
How long does the ACL take to heal?
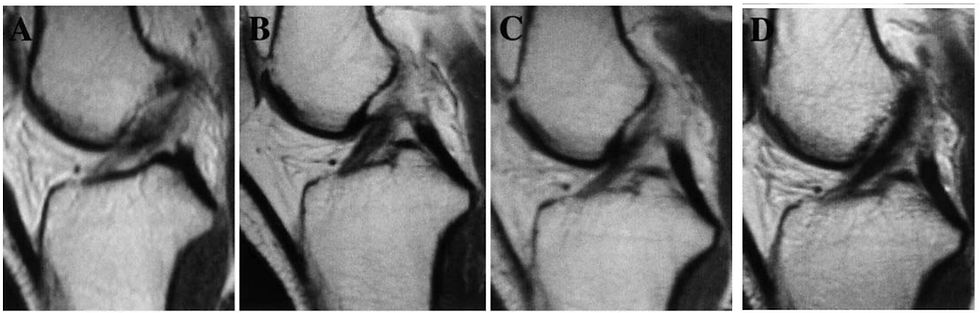
As with any injury, healing rates will vary on a range of individual factors. The Ihara (1994) study showed significant healing can occur in just 3 months. However, the below image from Ihara and Kawano (2017) study MRI taken on day 2 (A), 2 months (B), 6 months (C), 12 months (D), and 3 years (E) after injury, demonstrating that continued healing occurs at least 3 years after the initial rupture.

(Ihara and Kawano, 2017)
This research suggests that although initial healing can occur after a few months, rehabilitation should continue for many months, and even years, while healing continues to occur to improve the chances for a strong and stable knee.
What questions do we still have?
These papers challenge previous thinking, demonstrating that the ACL does have the ability to heal. However, we still have many questions to answer before we can confidently understand and advise on the self-healing process:
Do the changes increase with gender or age demographics? Do we need to brace the knee for a period (and in a specific position) following the injury? Which type of tear is more likely to heal (proximal vs mid-substance tears)? Is there a specific rehabilitation protocol that can positively influence healing rates? Is there an increased risk of re-rupture in self-healing compared to surgical repair? Are there new surgical options to promote the healing of ACL?
What's the take-home message?
These findings lay weight to the notion that not all ACL injuries require reconstructive surgery
We need at least 3 months (possibly longer) of high-quality rehabilitation to see if there are signs of ACL remodelling and repair
A full reassessment at 3 months post-injury should be completed, including full functional assessment and MRI scan
A delayed surgical reconstruction is a good option for many people following injury, particularly those with a reasonable level of function.
Need help with your ACL injury decision-making? Contact Tim or consider a telehealth consultation to discuss your ACL recovery.
References and Further Reading
Arnoczky SP. (1985) Blood supply to the anterior cruciate ligament and supporting structures. Orthop Clin North Am. Jan;16(1):15-28. PMID: 3969274.
Ferretti, A (2020) To Heal or Not to Heal: The ACL Dilemma. Journal of Orthopaedics and Traumatology, Aug, 21(11).
Filbay S, Roemer F, Lohmander S, et al. (2022) 32 Spontaneous healing of the ruptured anterior cruciate ligament: observations from the KANON trial. BMJ Open Sport & Exercise Medicine 2022;8:doi: 10.1136/bmjsem-2022-sportskongres.8
Filbay, S. R. and Grindem, H. (2019) ‘Evidence-based recommendations for the management of anterior cruciate ligament (ACL) rupture’, Best Practice and Research: Clinical Rheumatology. Elsevier Ltd, 33(1), pp. 33–47. doi: 10.1016/j.berh.2019.01.018.
Fujimoto, E, Sumen, Y, Ochi, M and Ikuta, Y (2002). Spontaneous Healing of Acute Anterior Cruciate Ligament (ACL) Injuries – Conservative Treatment Using an Extension Block Soft Brace Without Anterior Stabilization, Archives of Orthopaedic and Trauma Surgery, 122, 212-216.
Ihara H, Miwa M, Takayanagi K, Nakayama A. (1994) Acute torn meniscus combined with acute cruciate ligament injury. Second look arthroscopy after 3-month conservative treatment. Clin Orthop Relat Res. (307):146-54. PMID: 7924027.
Ihara, H and Kawano, T (2017). Influence of Age on Healing Capacity of Acute Tears the Anterior Cruciate Ligament Based on Magnetic Resonance Imaging Assessment, Journal of Computer Assisted Tomography, 41(2), 206-211.
Paterno, M. V. (2017) ‘Non-operative Care of the Patient with an ACL-Deficient Knee’, Current Reviews in Musculoskeletal Medicine. Current Reviews in Musculoskeletal Medicine, 10(3), pp. 322–327. doi: 10.1007/s12178-017-9431-6.
Van Meer, B, Oei, E, Bierma-Zeinstra, S, Van Arkel, E, Verhaar, J, Reijman, M and Meuffels, D (2014). Are Magnetic Resonance Imaging Recovery and Laxity Improvement Possible After Anterior Cruciate Ligament Rupture in Nonoperative Treatment?, Arthroscopy: The Journal of Arthroscopic & Related Surgery, Sept, 30(9), 1092-1099.

Comments